Though rare, and usually just a nuisance, this unique condition can have some strange symptoms.
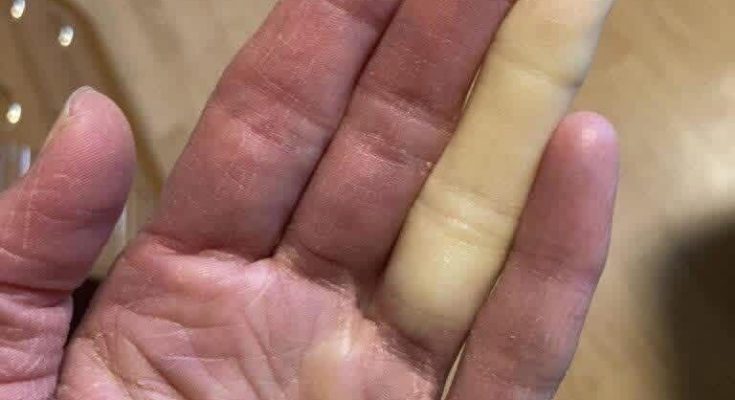
It’s a rather startling sight: You look down to see that your fingers—which you could swear were a healthy flesh tone just a second ago—have turned a rather stark shade of blue or maybe even white. But while it may be easy to chalk your skin’s color changes up to the temperature outside during colder months, if you notice it happening frequently, or say, whenever you grab a can of soda or are feeling particularly stressed, there might be more to it than just the weather.
Instead, says one expert, what you may be experiencing is something called Raynaud’s disease.
To get more information on this rather distinct condition, we turned to Sonali Narain, MD, a board-certified rheumatologist and director of the Scleroderma and Raynaud Treatment Center at Northwell Health.
What is Raynaud’s disease?
While Raynaud’s disease—also known as Raynaud’s phenomenon—most often describes the change of colors in a person’s hands from normal flesh tone to white, red, or blue following an exposure to cold, other areas of the body can be affected as well. “Sometimes this can also happen in a person’s feet, nose, and the earlobes,” explains Narain. This discoloration is caused by what is referred to as a vasospasm, or the narrowing of the blood vessels in an affected area, which occurs after skin comes into contact with something cold (think winter air, the refrigerator aisle at the supermarket, or a soda can).
“Having said that, not all Raynaud’s happens with cold exposure,” adds Narain. “It can also happen at room temperature in patients who have very severe disease, or in response to stress or certain medications.”
During an “attack,” blood vessels in the hand contract. This contraction limits blood flow to the fingers and causes discoloration in the skin. However, she explains, attacks are not just limited to color change. “There’s also discomfort that comes with it because you can have pain and burning and you can have numbness and tingling, too.”
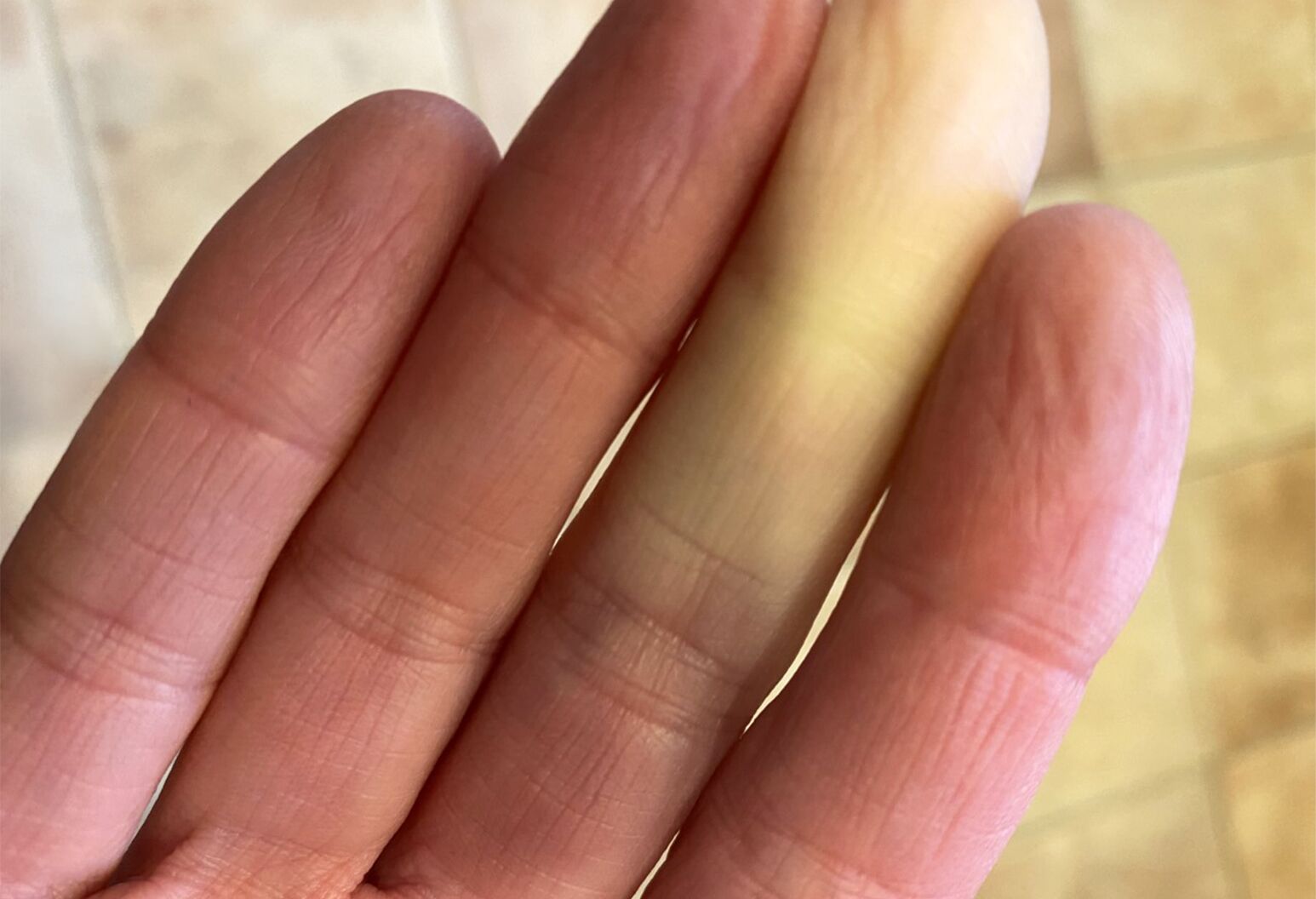
Who does Raynaud’s disease affect?
“A lot of patients will come in and describe their hands feeling very cold in the winter, or turning white when they were shoveling snow. But that’s not necessarily Raynaud’s,” explains Narain. “When someone actually has the disease, there’s a pretty dramatic shift in discoloration that happens.”
For those who do have Raynaud’s, the disease is classified in one of two ways.
The first is what’s referred to as primary Raynaud’s. “These are people who have a family history of Raynaud’s, where it probably existed in previous generations,” explains Narain. Beyond family history, she adds that certain medications, like birth control pills, which change the way our blood vessels behave, may also cause patients to experience the condition. Patients with primary Raynaud’s tend to skew on the younger side, with most diagnoses coming before the age of 30.
Like what you’re reading? Subscribe to our newsletter and get the same great content delivered straight to your inbox!
By providing your email address, you agree to receive email communication from The Well.
And, Narain adds, for these individuals, the condition tends to be pretty benign. “This means that most often, primary Raynaud’s will not get worse over time.”
The other form of the condition, referred to as secondary Raynaud’s, is most commonly diagnosed in patients who smoke, have had exposure to certain workplace chemicals, had previous injuries to the hands or feet, have an autoimmune condition, or have another medical condition that predisposes them to Raynaud’s. But while both primary and secondary Raynaud’s present in the same way—with distinctive discoloration of the skin—Narain says that for those with secondary Raynaud’s, there is a possibility of complications.
“It’s the patients with autoimmune conditions that we worry about—specifically those with scleroderma,” Narain says. “These patients tend to develop ulcers in their fingers because of lack of blood supply, which can lead to the dissolution of their bones and leave them with shortening of the digits.”
How do you treat Raynaud’s disease?
While roughly 5% of the U.S. population has Raynaud’s, for most people the condition amounts to little more than a nuisance.
“The most important thing is management,” says Narain. “So recognizing that you have the condition and doing everything that you can do to prevent these attacks.”
For those with Raynaud’s—both primary and secondary—prevention comes down to following a few measures:
- Use hand warmers
- Double glove in cold weather
- Use heaters in spaces—like offices—where you can’t control the temperature
- Reduce stress
- Limit caffeine intake
- Don’t smoke
- Avoid medications known to cause vasospasms (such as certain birth controls, blood pressure medications, and more)
In order to know which of your current medications may predispose you to Raynaud’s, Narain suggests consulting with your doctor to identify opportunities to switch medications where possible.
And if, after taking all of these steps, you’re still suffering from Raynaud’s attacks, then a conversation with your doctor may be in order. “So if you’ve done your due diligence and you’re still having episodes of symptoms, then we go to medications that help improve blood circulation to avoid these attacks,” explains Narain.