Acute generalized exanthematous pustulosis is a rare severe cutaneous adverse reaction that classically presents in intertriginous or flexural areas and subsequently spreads diffusely across the trunk and extremities. To date, few cases of acute generalized exanthematous pustulosis arising in a photodistributed pattern are documented. Herein, we describe the second known case of photodistributed generalized exanthematous pustulosis arising in association with oral terbinafine use, providing a summary of the previously documented cases along with exploration of the potential pathophysiological mechanisms for this cutaneous reaction.
Introduction
Acute generalized exanthematous pustulosis (AGEP) is a severe cutaneous adverse reaction (SCAR) characterized by non-follicular, sterile pustules overlying confluent erythema. Overwhelmingly, most cases are drug-induced with antibiotics, antifungals, antimalarials, anticonvulsants, analgesics, and calcium channel blockers implicated as the major causative agents.1–4 Classically, AGEP arises in intertriginous sites and generalizes to the trunk and extremities.1,2 Patients may experience fever and lab abnormalities, including leukocytosis, neutrophilia, eosinophilia, hypocalcemia, transaminitis, elevated creatinine, and elevated C-reactive protein (CRP).1–3 Herein, we present a case of terbinafine-induced, photodistributed AGEP.
Case
A 48-year-old female presented for an eruption beginning 8 days after initiation of oral terbinafine. While taking the medication, she traveled to the beach and had frequent sun exposure. While on vacation, she noted a pruritic, red rash in her inguinal creases, which quickly spread to her trunk and extremities. She denied prior use of terbinafine.
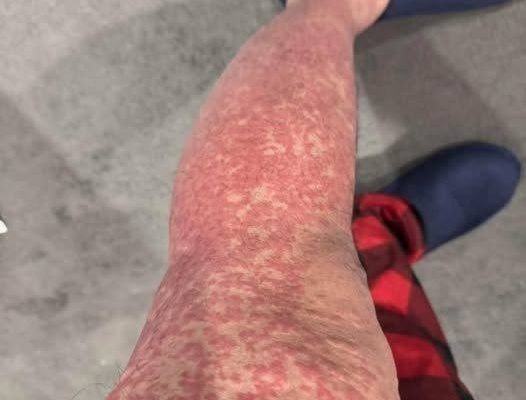
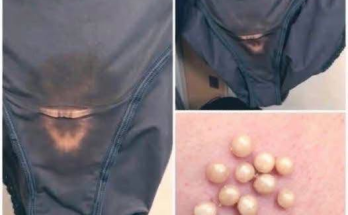
On examination, erythematous papules and plaques were noted diffusely on the trunk and extremities with clusters of small, non-follicular pustules on the arms and chest in a photodistributed pattern with sharp demarcation at areas covered by clothing (Figures 1–3). Laboratory studies were significant for neutrophilic leukocytosis, elevated CRP, and mild uncorrected hypocalcemia. Biopsy showed epidermal acanthosis and spongiosis with subcorneal pustules and dense dermal inflammation with eosinophils and neutrophils (Figures 4 and 5). Based on these findings, the patient was diagnosed with AGEP with a EuroSCAR score of 9.1 She improved with a 5-day course of intravenous dexamethasone and twice daily application of betamethasone dipropionate 0.05% ointment. After 1 week, all pustules resolved with residual desquamation.





Discussion
Putatively, a drug-specific T-cell mediated type IV hypersensitivity reaction typifies AGEP.5 The formation of pustules is driven by activation of innate and reactive immune responses. Specifically, upon exposure to the inciting agent, drug-specific T-cells migrate to the skin, leading to production of numerous cytokines and chemokines. T-cell–derived C-X-C motif chemokine ligand 8 (CXCL8) recruits neutrophils to lesional skin, while granulocyte-macrophage colony-stimulating factor prevents apoptosis of recruited neutrophils, supporting their accumulation.2,5,6 Upregulation of interleukins (IL) such as IL-17 and IL-22 stimulate keratinocyte production of additional CXCL8 and IL-8, synergistically contributing to chemotaxis and amassment of neutrophils in the stratum corneum and epidermis, as observed in lesional AGEP tissue specimens.5,6 Production of additional inflammatory cytokines such as tumor necrosis factor-alpha, IL-1, IL-6, IL-12, and IL-23 further augment recruitment and activation of neutrophils.5 A genetic predisposition may underpin the development of AGEP as human leukocyte antigens B51, DR11, and DQ3 are more frequently observed in patients with AGEP.7 Moreover, mutations in the IL-36RN gene, encoding the IL-36 receptor antagonist, may be responsible for the increased downstream production of IL-1, IL-6, and IL-8.5,6 However, the role of ultraviolet (UV) in triggering or exaggerating AGEP has not been established.
AGEP arising in a photo-distributed or photo-accentuated pattern is rare, with only a few existing reports in the medical literature attributed to hydroxychloroquine-psoralen plus ultraviolet-A light therapy, sertraline, liraglutide, and antimicrobials, as outlined in Table 1, leading some to refer to this entity as acute photodistributed exanthematous pustulosis.8–14 Our case further supports UV exposure as a potential exacerbating factor for terbinafine-induced AGEP.