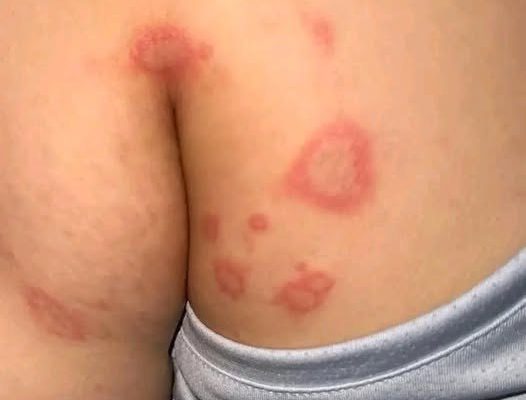
An 89-year-old White woman presents to her primary care provider (PCP) with an erythematous, flat, patchy rash on both forearms that has been present for about 10 days (Figure 1). The PCP diagnoses the rash as a photosensitivity rash following the attendance of an outdoor airshow 2 weeks prior. Triamcinolone cream is prescribed, and the rash fades slightly over 2 to 3 weeks with regular use.

A month later, the patient returns to the PCP with an extremely pruritic rash that began on her back and has quickly spread to her trunk. The rash has progressively worsened despite reapplying the triamcinolone cream to the rash for 1 week without relief. She denies the use of new detergents, soaps, topical creams, food, medication, or new clothing. She has not traveled, been around sick contacts, or had any known insect bites.
She denies fever, chills, fatigue, weight loss, oral or nasal ulcers, dry mouth, swollen lymph nodes, dyspnea, chest pain, edema, nausea, vomiting, diarrhea, joint swelling, muscle aches, or numbness.
The patient’s medical history is significant for coronary artery disease with stent placement in 2017, aortic valve replacement in 2015, hypertension, hyperlipidemia, hypothyroidism, osteoarthritis, and osteoporosis. Her medical conditions are well controlled on medications, which have been consistent since 2017, and include atorvastatin (80 mg every night at bedtime), enalapril (2.5 mg/d), metoprolol (25 mg/d), levothyroxine (75 mcg/d), clopidogrel (75 mg/d), and subcutaneous denosumab (60 mg every 6 months). Her immunizations are up to date, including COVID-19, influenza, shingles, and pneumonia.
She has been widowed for 10 years and lives independently, prepares her own meals, and needs no assistance with medications. She does not drink alcohol, smoke, or use illicit drugs, and plays Rummikub with friends in her community several nights during the week. Her 3 adult children live nearby, visit regularly, drive her to medical appointments, and assist with grocery shopping and household chores.
Physical Examination
Physical examination reveals a pleasant older woman in no acute distress. She is awake, alert, and oriented to person, place, and time. The skin of her neck, chest, and arms presents with diffuse erythematous, raised, slightly scaled lesions with distinct edges, measuring approximately 3 cm to 4 cm, with no surrounding erythema. There are strikingly annular and hemi-annular erythematous lesions measuring 4 cm to 5 cm over the back, buttocks, and a few on the upper arms (Figure 2). No lesions are observed on the face or in the mouth or nose. The distal interphalangeal joints bilaterally reveal Heberden nodes but no erythema or swelling of any other joints. Heart and lung examinations are unchanged from baseline.

Differential Diagnosis
The differential diagnosis includes multiple cutaneous conditions that commonly present with erythematous, annular dermatologic lesions, such as erythema migrans, plaque psoriasis, granuloma annulare, erythema annulare centrifugum (EAC), pityriasis rosea, erythema multiforme, polymorphic light eruption, secondary syphilis, dermatomyositis, T-cell lymphoma, tinea corporis, lichenoid photo drug eruption, Lyme disease, and pemphigus foliaceus.1 Among these, the initial differentials are Lyme disease, EAC, and tinea corporis.2
Diagnostic Workup/Diagnosis
A Lyme titer is drawn at the first visit and was negative. Initial treatment with high-potency topical steroids and antifungals is not fruitful in resolution of the rash. The rash remains extensive and non-remitting, so the patient is referred to dermatology for consultation. A skin biopsy is performed 10 days after the initial primary care visit. Biopsy results include dermoepidermal junction smudging, interface dermatitis, and evidence of subacute cutaneous lupus erythematosus (SCLE) and drug eruption. Upon biopsy results, the patient’s enalapril was suspected as the offending agent and stopped immediately. The patient was started on a 16-day tapering dose of prednisone starting at 40 mg and ending with 5 mg, which improveds symptoms, but the rash returned within 2 weeks of prednisone cessation (Figures 3 and 4).


A second dermatologist is consulted for a second opinion 1 month later and performs laboratory testing. Skin biopsy and laboratory testing confirmed the patient’s diagnosis of drug-induced SCLE (DI-SCLE; Table).

Treatment and Disease Course
A rheumatologist is consulted and the patient is prescribed oral hydroxychloroquine 200 mg and 400 mg, to be taken on alternating days. Despite slight rash improvement, the medication was discontinued after 2 weeks because of adverse effects of diarrhea and nausea. Prednisone is restarted at 5 mg daily, and after 30 days, is lowered to a daily dose of 1 mg, which became the long-term regimen. Since diagnosis and treatment the patient has dramatically improved, but experiences occasional plaque formation that resolves with topical betamethasone. She now avoids direct sunlight, is back to playing Rummikub with her friends, is adherent with medications, and living life.
Discussion
Subacute cutaneous lupus erythematosus is a form of cutaneous lupus erythematosus that presents with erythematous, annular plaques or papulosquamous drug-related eruption in sun-exposed areas.2,3 The lesions typically occur in the V-neck area of the chest, back, shoulders, extensor sides of the upper extremities, and can extend to the face, scalp, and legs.4 Most patients with DI-SCLE are White women, with a mean age of 60 years.5,6 SCLE can be idiopathic (I-SCLE) or drug-induced (DI); both types have the same immunologic and histopathologic findings and are difficult to distinguish clinically.7
Since the first reported case of DI-SCLE in 1985, more than 50 medications have been implicated in this disorder, many associated with induction of photosensitivity reactions.3,8 In addition to proton pump inhibitors (PPI), nonsteroidal anti-inflammatory drugs (NSAIDs), chemotherapeutics, and anti―tumor necrosis factor (TNF) agents, the most common drugs correlated with DI-SCLE fall under the antihypertensive umbrella, particularly thiazides, beta-blockers, angiotensin-converting enzyme (ACE) inhibitors, and calcium channel blockers. Other agents that have been implicated as a cause of DI-SCLE include carbamazepine, interferon alfa and beta, leflunomide, simvastatin, and terbinafine.2,3,8 Antihypertensives and antiepileptics have the longest incubation period, with a median time of 2 years’ use before SCLE symptoms appear.9
Patient medication profiles inclusive of several known causative agents implicated in DI-SCLE can complicate the diagnostic and treatment process. Although statins have also been found to cause DI-SCLE, in this case, the rash improved when enalapril was discontinued.
Research has found the age of disease onset to be higher in patients with DI-SCLE compared with I-SCLE. This is hypothesized to correlate with the increased use of medications with age.10 Thorough history taking and detailed attention to medication lists can aid in diagnosis.8
The laboratory findings include the presence of anti-Ro/SSA (Sjögren syndrome-A) and or anti-La/SSB (Sjögren syndrome-B) together with antinuclear antibodies (ANA) and antihistone antibodies.2,11 In this case, the patient was positive for ANA and anti-Ro/SSA, while negative for anti-La/SSB. Diagnosis can become complicated when there is pre-existing lupus and prior evidence of positive autoantibodies and serologies, as there are no additional formal diagnostic criteria for DI-SCLE.8
The incubation period for a DI reaction can be anywhere from 3 days to 11 years, with a median latency of 6 weeks.2 The diagnosis of DI-SCLE is usually made when one of the common medications known to cause the rash is taken prior to the eruption, and improves when the medication is stopped.3,10,12 The cornerstone of DI-SCLE treatment is identification and discontinuation of the suspected causative medication, which usually results in symptom resolution within 8 to 12 weeks.3,8,10 In the event of continued symptoms, the most common medications in the literature to treat DI-SCLE are topical steroids, oral prednisone, and the immunosuppressive drugs hydroxychloroquine and oral tacrolimus.3
Conclusion
Although DI-SCLE is relatively uncommon and often misdiagnosed, the root cause is likely a photosensitivity reaction from medications most commonly prescribed by PCPs. With careful history taking and attention to details of medication lists, particularly new medications prescribed for patients older than 60, identification of this disorder can occur on the front line. Withdrawal of suspected offending medications can promote resolution and prevent patients from enduring extended symptoms while awaiting specialist referrals and undergoing costly lab work and invasive tests for diagnosis. In this case, primary care referrals to dermatology and rheumatology helped make the correct diagnosis and treat the disease, limiting the patient’s side effects and hastening resolution.
- Lazar AL. Subacute cutaneous lupus erythematosus: a facultative paraneoplastic dermatosis. Clin Dermatol. 2022;40(6):728-742. doi:10.1016/J.CLINDERMATOL.2022.07.007
- Mizuta T, Kato M. Amlodipine-induced subacute cutaneous lupus erythematosus localized to non-sun-exposed areas. Case Rep Dermatol. 2022;14(1):71-76. doi:10.1159/000524001
- Gray T, Segars K, Farsi M, Ross R, Miller R. Drug-induced anti-Ro positive subacute cutaneous lupus in a man treated with olmesartan. Dermatol Online J. 2019;25(12). doi:10.5070/D32512046719
- Callen JP. Drug-induced subacute cutaneous lupus erythematosus. Lupus. 2010;19(9):1107-1111. doi:10.1177/0961203310370349
- Dalle Vedove C, Simon JC, Girolomoni G. Drug-induced lupus erythematosus with emphasis on skin manifestations and the role of anti-TNFα agents. J Dtsch Dermatol Ges. 2012;10(12):889-897. doi:10.1111/J.1610-0387.2012.08000.X
- Borucki R, Werth VP. Cutaneous lupus erythematosus induced by drugs – novel insights. Expert Rev Clin Pharmacol. 2020;13(1):35-42. doi:10.1080/17512433.2020.1698290
- Aggarwal N. Drug-induced subacute cutaneous lupus erythematosus associated with proton pump inhibitors. Drugs Real World Outcomes. 2016;3(2):145-154. doi:10.1007/S40801-016-0067-4
- Keyes E, Grinnell M, Vazquez T, Diaz DA, Thomas P, Werth VP. Drug-induced subacute cutaneous lupus erythematosus in previously diagnosed systemic lupus erythematosus patients: a case series. JAAD Case Rep. 2021;12:18-21. doi:10.1016/J.JDCR.2021.03.048
- Laurinaviciene R, Sandholdt LH, Bygum A. Drug-induced cutaneous lupus erythematosus: 88 new cases. Eur J Dermatol. 2017;27(1):28-33. doi:10.1684/EJD.2016.2912
- Guicciardi F, Atzori L, Marzano AV, et al. Are there distinct clinical and pathological features distinguishing idiopathic from drug-induced subacute cutaneous lupus erythematosus? A European retrospective multicenter study. J Am Acad Dermatol. 2019;81(2):403-411. doi:10.1016/j.jaad.2019.02.009
- Patel NB, Cuervo-Pardo L, Tan TL, Kundu RV, Chiarella SE. Proton pump inhibitor–induced subacute cutaneous lupus erythematosus. J Allergy Clin Immunol Pract. 2020;8(1):326-327. doi:10.1016/j.jaip.2019.07.025
- Bui AN, Hirner J, Singer SB, et al. De novo subacute cutaneous lupus erythematosus-like eruptions in the setting of programmed death-1 or programmed death ligand-1 inhibitor therapy: clinicopathological correlation. Clin Exp Dermatol. 2021;46(2):328-337. doi:10.1111/CED.14449